Patient is a 50 year old male who came in August 2014 complaining of left hip pain. Prior to this visit the patient had a left hip replacement in May 2013, performed by Orthopedic Surgeons at an alternative facility.
Patient had come in complaining of severe pain, which he felt had been increasing since his surgery in May 2013.
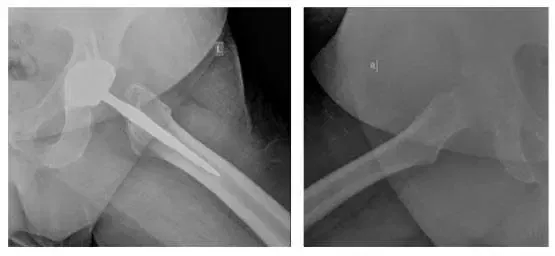
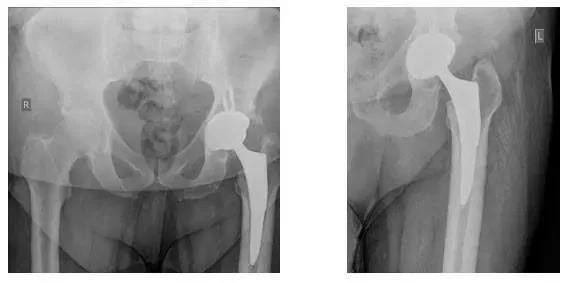
X-rays of Bilateral Hips. Four views were taken: AP Pelvis (top left), Left AP Hip (top right), Left Lateral Frog (bottom left), Right Lateral Frog (bottom right).
X-rays reveal osteolysis in the acetabulum with possible loosening of the femoral component. Loosening is best seen on comparison with earlier X-ray.
Options were discussed with the patient along with the increased risks that can be associated with revision hip surgery. A few of the risks discussed consisted of, but are not limited to, infection, deep various thrombosis, stiffness, loosening of the implant, persistent worsening of pain, nerve or vascular injury, healing possibly requiring transfusion, loss of sensation, instability, and mortality.
The doctor requested for an op report while the patient was advised to get an aspiration of the left hip to test for cell count with differential, culture, and sensitivity – aerobic, anaerobic and acid fast; the patient was also informed to not take any antibiotics for at least 2 weeks before getting the aspiration.
The patient was also advised to obtain a left hip CT scan and obtain metabolic bone labs which included 25-hydroxy Vitamin D. The patient then followed up to review the results of the tests. The aspiration had indicated that the patient was positive with MRSA in his nares and had an infected D/T joint prosthesis.
Results also revealed that the patient had a high ESR and a high cell count. The patient was informed that the best approach for him would be a staged reconstruction, which the patient had chosen to proceed with.
The Left Hip THA was performed on 10/13/2014.
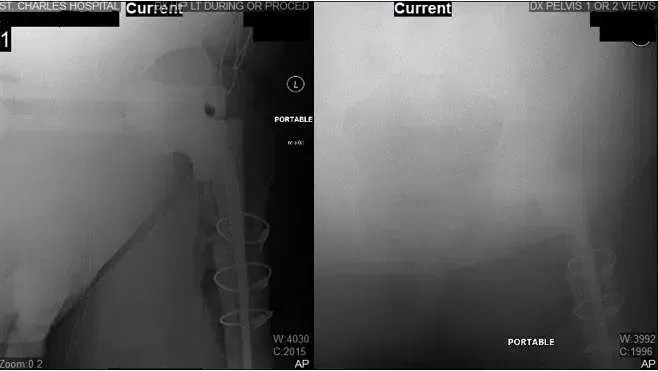
X-Ray of Left Hip during operation. X-Rays show Left Hip Replacement.
The patient followed-up 6 weeks after his spacer spacer placement surgery and brought new X-rays to review. At this point, post-op, the patient’s scar had healed well and he had moderately restricted range of motion. However, due to the MRSA in his nares, the patient was advised to get a left hip aspiration and to follow up with the results, while also continuing antibiotics per ID.
Upon follow up, revision surgery was discussed with the patient as well as all of the risks, benefits, and any alternative options. The patient understood the underlying risks associated, including, but not limited to, the ones previously stated.
The Removal of Spacer and Revision of Left Hip THA was performed on 1/15/2015.
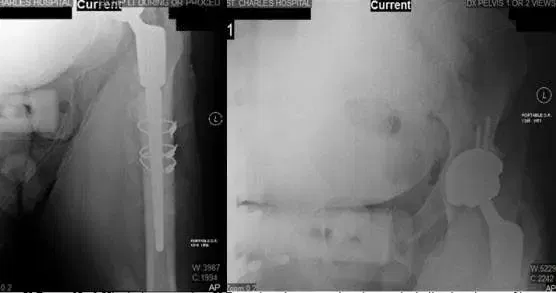
X-Rays of Left Hip during operation.
X-Rays show intraoperative changes including instalment of long stem THA, 2 screws setting the acetabulum, and cerclage wires surrounding the femur. X-Rays also show a nondisplaced transverse fracture of the proximal one-third femoral shaft.
The patient followed-up about 4 weeks post Removal of Spacer and Revision Left THA with new X-rays to review. The patient presented with a moderate restriction of his range of motion, decreased strength, and atrophy.
He was advised to continue taking Aspirin 325mg two times a day, Vitamin D3 5,000 IU daily, and to follow up in 6 weeks with new X-rays to monitor progression post-operatively.
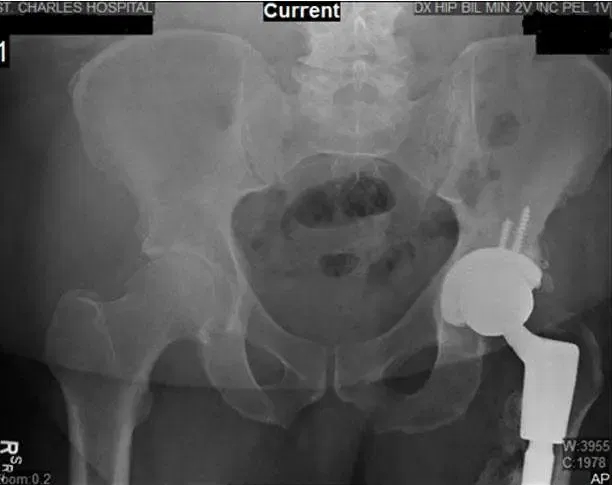
X-Ray of Bilateral Hip. X-ray shows Left THA along with new bone formation along the lateral and proximal shaft of the femur.
The patient had stated that he was feeling good relief from the pain medication. Upon examination, he was experiencing tenderness over the greater trochanter of both the lower left and lower right extremities. At subsequent follow-ups the X-rays reviewed were normal and showed that there was no acute displaced fracture and possible focal osteopenia of the loosening. The patient was advised to begin weight bearing as tolerated and continue Vitamin D3 5,000 IU daily.
Patient then came in 6 weeks later for a follow-up and presented with minimal stiffness and start up. He was instructed to continue previous treatment plan including continue the Vitamin D3 5,000 IU daily and weight bearing as tolerated. The patient has done very well subsequently.

Proximal segment of the modular femoral component
The proximal component is shown in the image above fits in the distal stem (image below). Together they form the modular femoral component for revision/complex hip replacement surgery. The modularity allows the surgeon to make intraoperative changes to achieve greater stability and function.

The distal stem of the modular femoral component
*Patient identifiers and dates changed to protect patient privacy.





